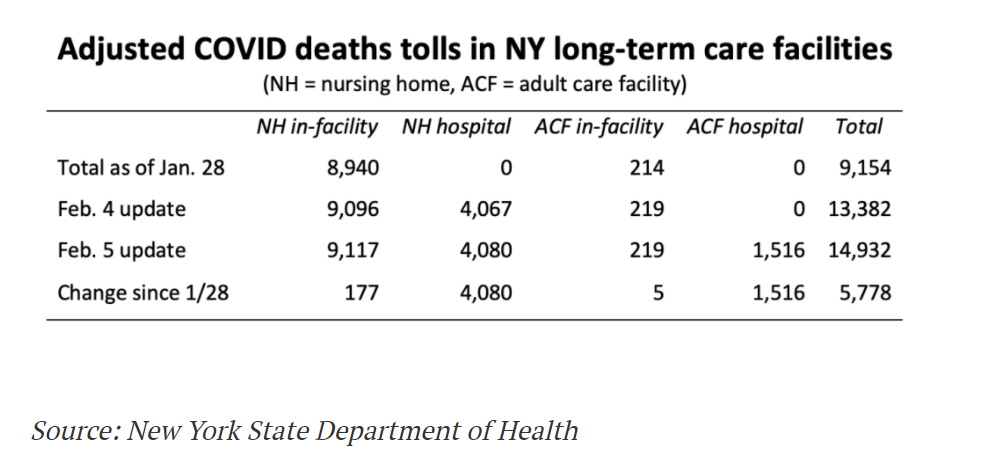
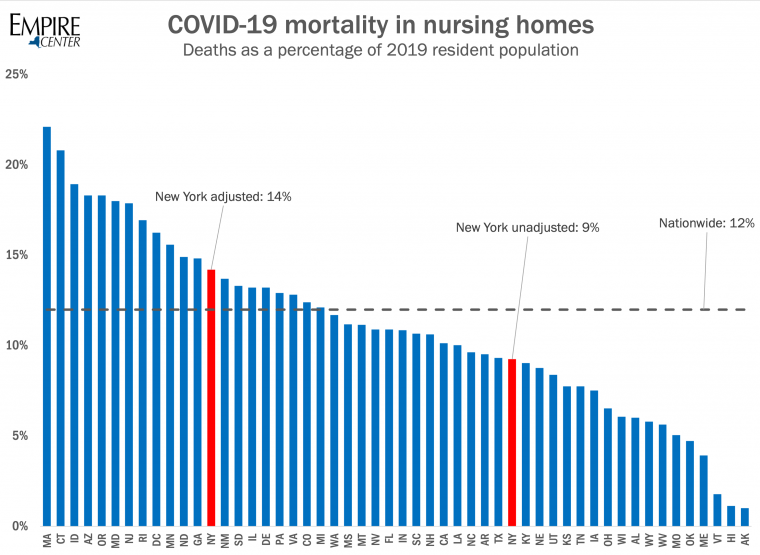
Graphic:
Excerpt:
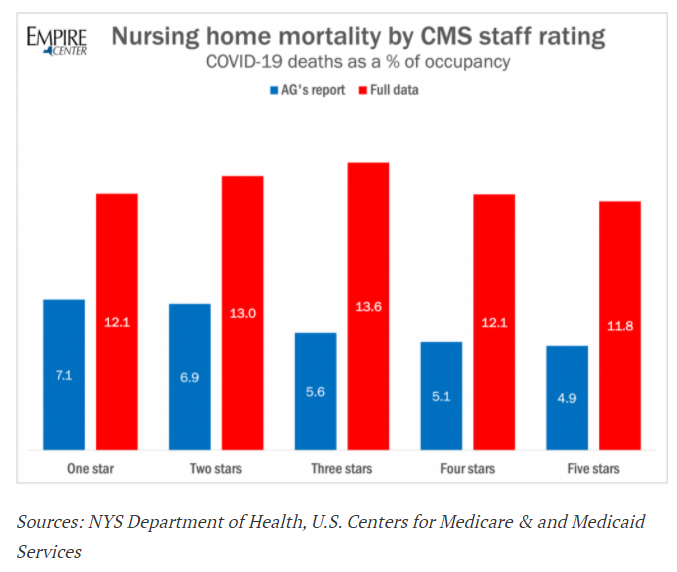
In its January 28 report, the attorney general’s office argued that low staffing levels in nursing homes was associated with higher death rates from the novel coronavirus. As evidence of that connection, the report presented a table (reproduced in Table 1 below) comparing death rates in nursing homes based on their star ratings for staffing from the U.S. Centers for Medicare & Medicaid Services (CMS).[5] It showed that homes with the lowest staffing grade of one star had an aggregate COVID-19 mortality rate of 7.13 percent, compared to 4.94 percent for homes with a five-star rating.
However, that table was based on the limited data available in mid-November, which encompassed 6,645 deaths, only half the number that are documented now.
When that table is brought up to date, it shows no clear association between lower staffing grades and higher coronavirus mortality (see Table 2). Homes with a three-star staff rating showed the largest percentage of deaths, at 13.62, compared to 12.98 for two-star homes and 12.14 for one-star homes.[6]
Author(s): Bill Hammond, Ian Kingsbury
Publication Date: 4 March 2021
Publication Site: Empire Center for Public Policy