Link: https://www.scientificdiscovery.dev/p/20-so-many-great-things-you-missed
Graphic:
Excerpt:
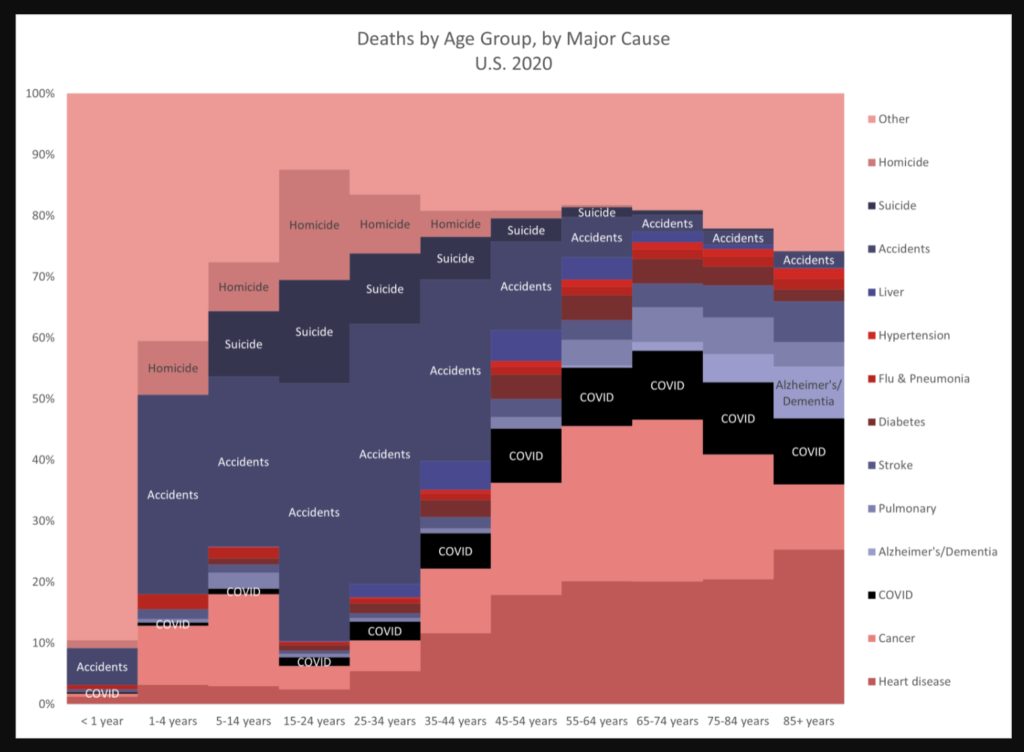
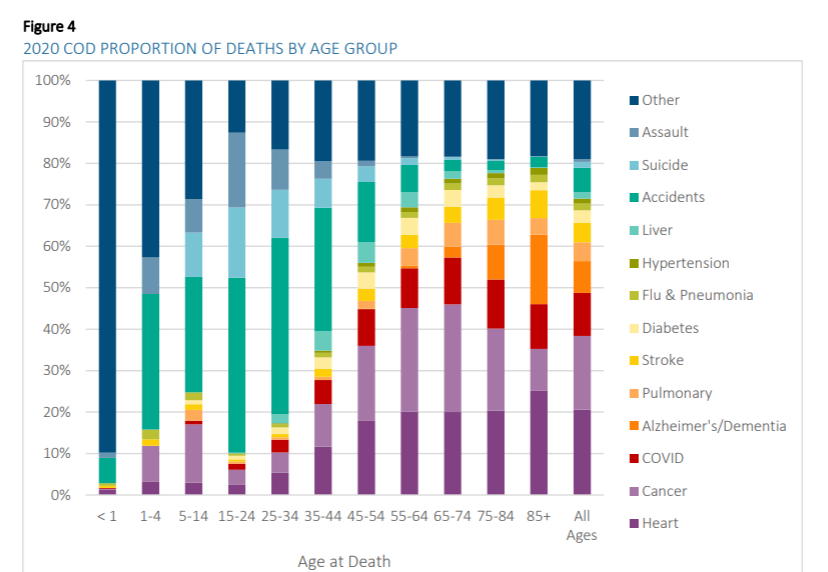
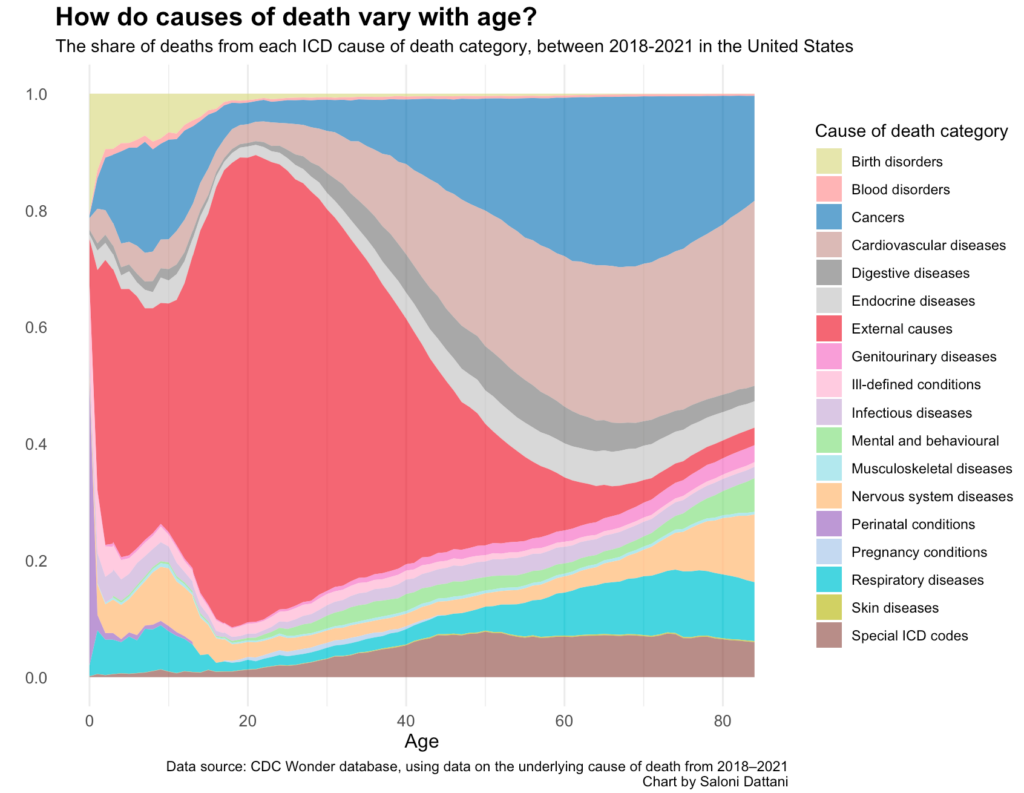
You can see that, in childhood, in the US, the most common causes of death are ‘external causes’. This is a broad category that includes accidents, falls, violence, and overdoses, and is shown in red. But there’s also a notable contribution from birth disorders (in muted green), childhood cancers (in blue), and respiratory diseases (in cyan).
The share of deaths in childhood from cancers stood out to me. We’ve seen lots of progress against many childhood cancers over the last 50 years — notably in treating leukemia, brain cancers, kidney cancers, lymphomas, and retinoblastoma — but this is a reminder that there’s still further to go.
From adolescence until middle-age, ‘external causes’ are now the overwhelming cause of death. Around 80% of deaths at the age of 20 in the US are due to external causes. These result from causes such as accidents, violence, and overdoses.
At older ages, diseases rise in importance. Causes of death also become more varied, although cardiovascular diseases and cancers are the most common.
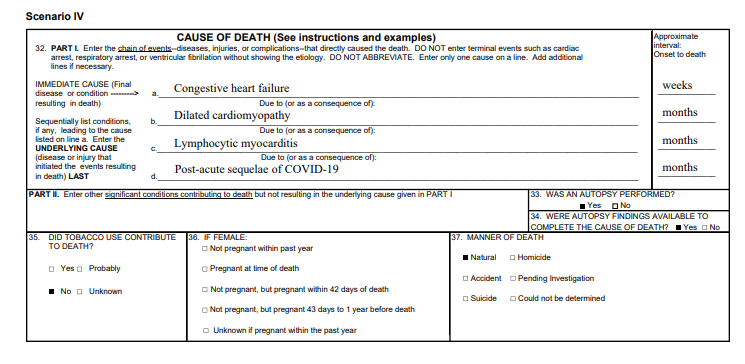
You might also be wondering about the brown category at the bottom, called ‘special ICD codes’. That’s a placeholder category in the system for deaths caused by new diseases — predominantly Covid-19, since the data spans 2018 to 2021.3
Author(s): SALONI DATTANI
Publication Date: 16 Mar 2022
Publication Site: Scientific Discovery on substack