Link: https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm
Graphic:
Excerpt:
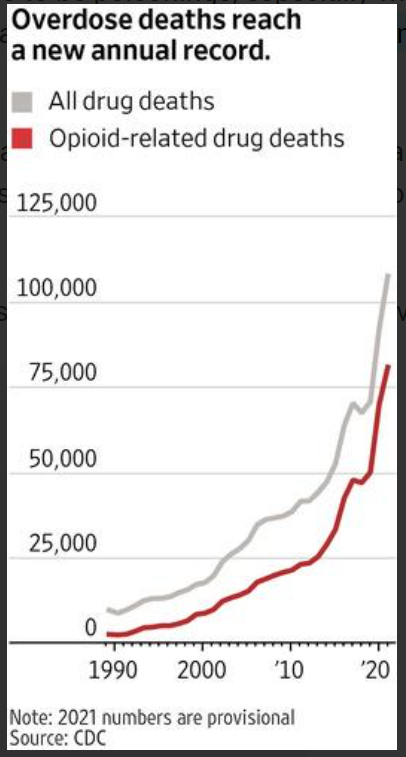
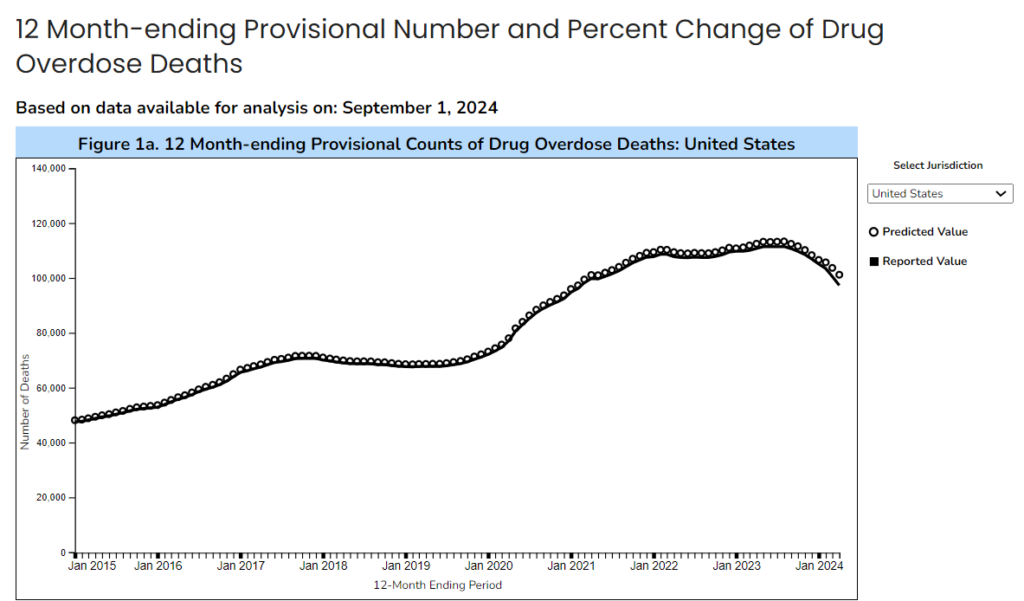
This data visualization presents provisional counts for drug overdose deaths based on a current flow of mortality data in the National Vital Statistics System. Counts for the most recent final annual data are provided for comparison. National provisional counts include deaths occurring within the 50 states and the District of Columbia as of the date specified and may not include all deaths that occurred during a given time period. Provisional counts are often incomplete and causes of death may be pending investigation (see Technical notes) resulting in an underestimate relative to final counts. To address this, methods were developed to adjust provisional counts for reporting delays by generating a set of predicted provisional counts (see Technical notes).
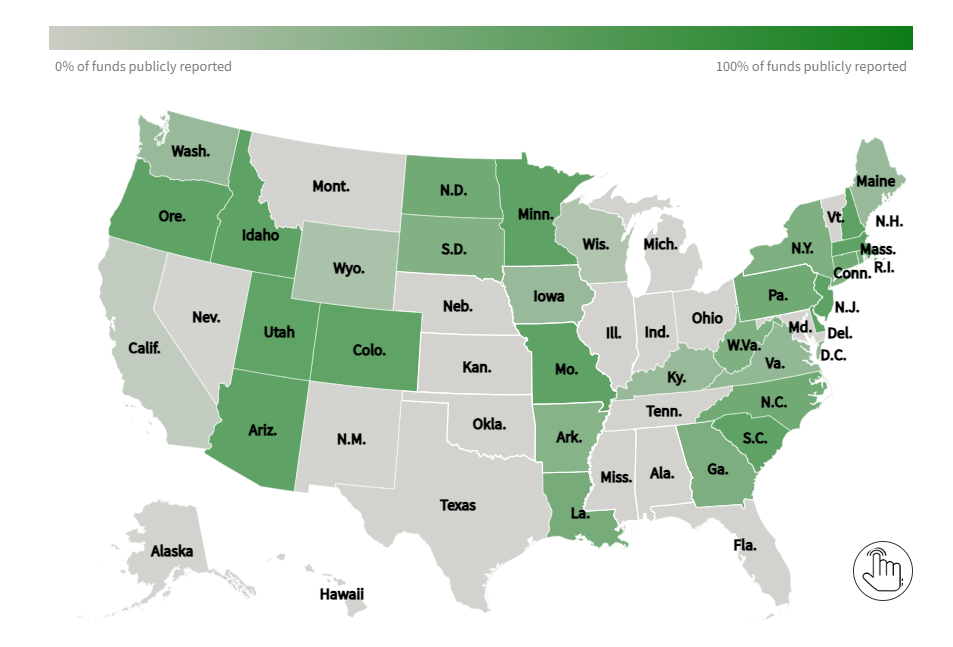
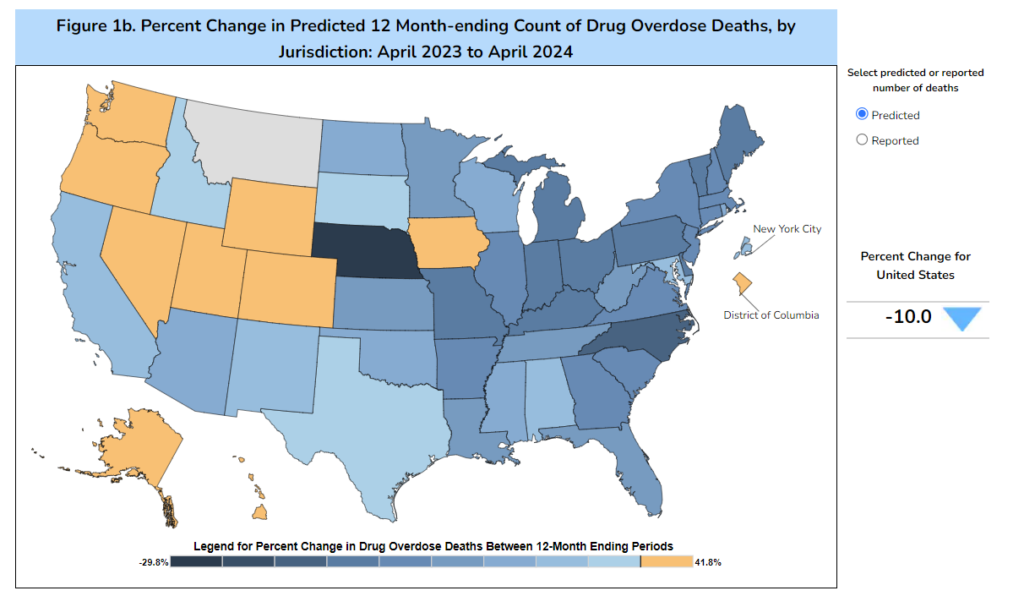
The provisional data presented in this visualization include: (a) the reported and predicted provisional counts of deaths due to drug overdose occurring nationally and in each jurisdiction; (b) a U.S. map of the percentage changes in provisional drug overdose deaths for the current 12 month-ending period compared with the 12-month period ending in the same month of the previous year, by jurisdiction; and (c) the reported and predicted provisional counts of drug overdose deaths involving specific drugs or drug classes occurring nationally and in selected jurisdictions. The reported and predicted provisional counts represent the numbers of deaths due to drug overdose occurring in the 12-month periods ending in the month indicated. These counts include all seasons of the year and are insensitive to variations by seasonality. Deaths are reported by the jurisdiction in which the death occurred.
Several data quality metrics, including the percent completeness in overall death reporting, percentage of deaths with cause of death pending further investigation, and the percentage of drug overdose deaths with specific drugs or drug classes reported are included to aid in interpretation of provisional data as these measures are related to the accuracy of provisional counts (see Technical notes). Reporting of the specific drugs and drug classes involved in drug overdose deaths varies by jurisdiction, and comparisons of death rates involving specific drugs across selected jurisdictions should not be made (see Technical notes). Provisional data presented in this visualization will be updated on a monthly basis as additional records are received.
Publication Date: Accessed 19 Sept 2024
Publication Site: National Center for Health Statistics, CDC