Link: https://jamanetwork.com/journals/jama-health-forum/fullarticle/2802095
JAMA Health Forum. 2023;4(3):e230010. doi:10.1001/jamahealthforum.2023.0010
Graphic:
Excerpt:
Key Points
Question Do postacute sequelae of SARS-CoV-2 increase risks of 1-year adverse outcomes?
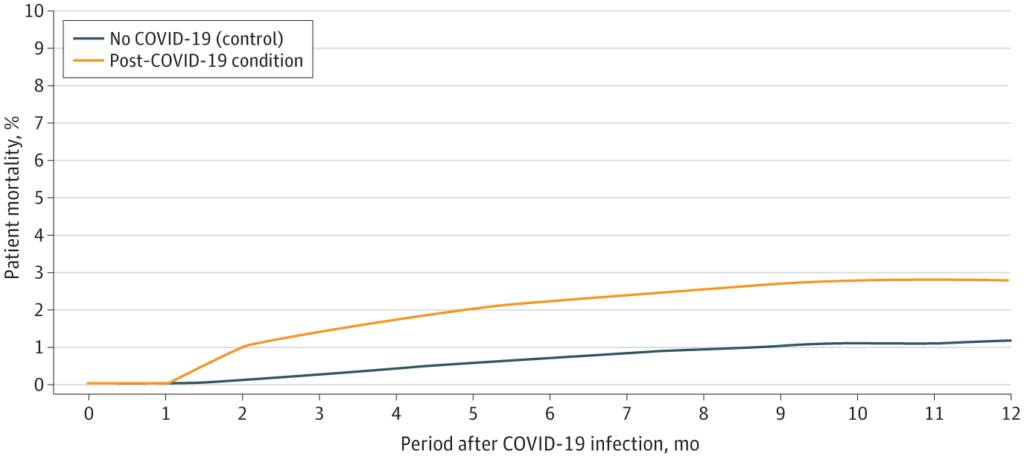
Findings In this case-control study of 13 435 US adults with post–COVID-19 condition (PCC) and 26 870 matched adults without COVID-19, the adults with PCC experienced increased risks for a number of cardiovascular outcomes, such as ischemic stroke. During the 12-month follow-up period, 2.8% of the individuals with PCC vs 1.2% of the individuals without COVID-19 died, implying an excess death rate of 16.4 per 1000 individuals.
Meaning Individuals with PCC may be at increased risk for adverse outcomes in the year following initial infection.
Author(s): Andrea DeVries, PhD1; Sonali Shambhu, BDS, MPH1; Sue Sloop, PhD1; et al
Publication Date:
Publication Site: JAMA Health Forum