`
Link:https://www.statnews.com/2023/11/07/pulse-oximeters-attorneys-general-urge-fda-action/
Excerpt:
More than two dozen attorneys general are urging Food and Drug Administration officials to take urgent action to address disparities in how well pulse oximeters, the fingertip devices used to monitor a person’s oxygen levels, work on people with darker skin.
In a Nov. 1 letter, the AGs noted that it had been a year since the FDA convened a public meeting of experts, who called for clearer labeling and more rigorous testing of the devices, and that no action had been taken.
“We, the undersigned Attorneys General, write to encourage the FDA to act with urgency to address the inaccuracy of pulse oximetry when used on people with darker toned skin,” said the letter, written by California Attorney General Rob Bonta and signed by 24 other attorneys general.
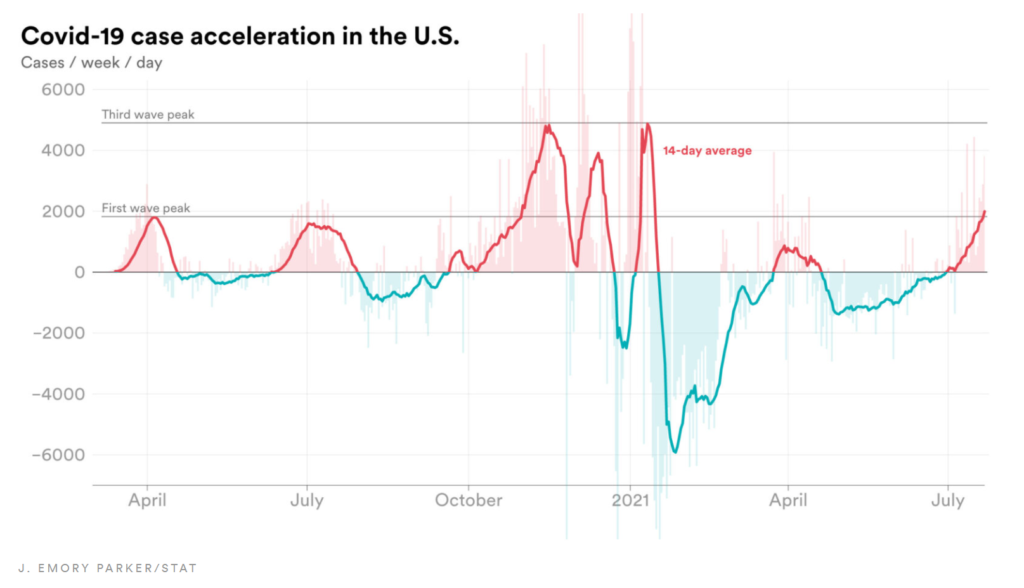
Pulse oximeters’ overestimation of oxygen levels in patients with darker skin has, in a slew of recent research studies, been linked to poorer outcomes for many patients because of delayed diagnosis, delayed hospital admissions, and delayed access to treatment, including for severe Covid-19 infections. Higher amounts of pigments called melanin in darker skin interfere with the ability of light-based sensors in pulse oximeters to detect oxygen levels in blood.
….
The delay has frustrated health care workers who use pulse oximeters and have studied them and followed the progress toward creating new devices that work better. “I just get mad that these things are not on the market,” Theodore J. Iwashyna, an ICU physician at Johns Hopkins, told STAT. “Just last week in my ICU, I had a patient whose pulse oximeter was reading 100% at the same time that his arterial blood gas showed that his oxygen levels were dangerously low. I need these things to work, and work in all my patients.”
Author(s):Usha Lee McFarling
Publication Date: 7 Nov 2023
Publication Site: STAT News