Graphic:
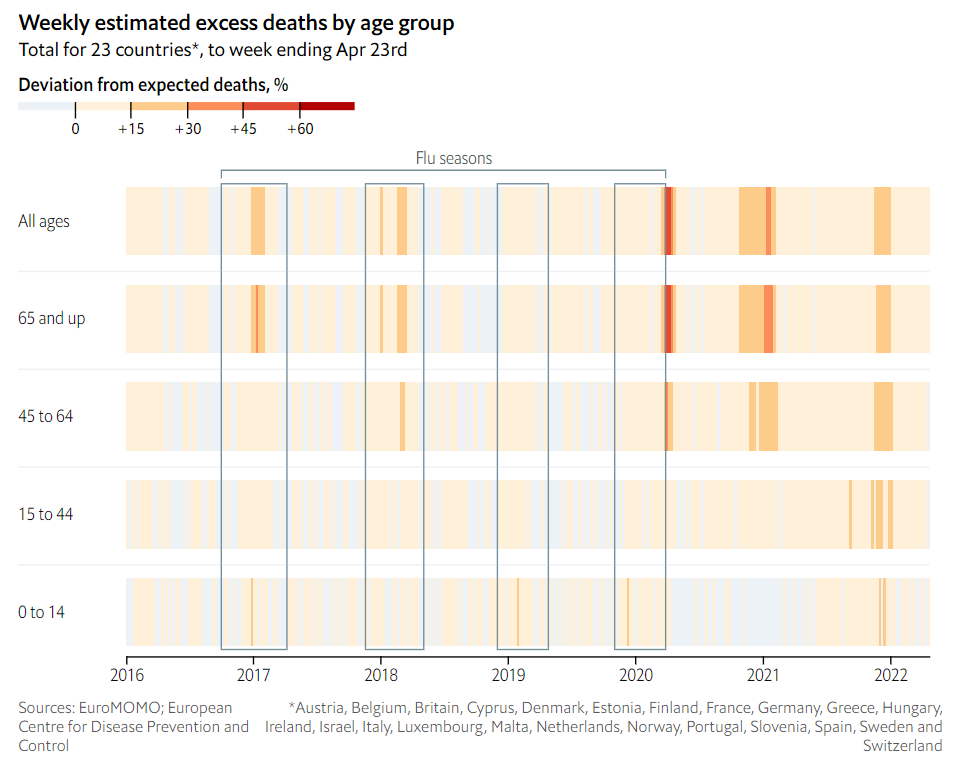
Excerpt:
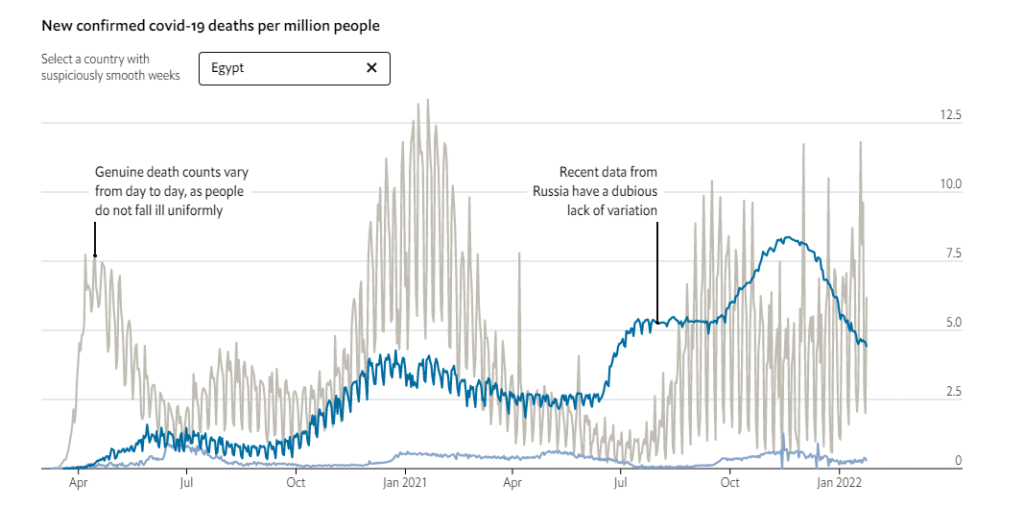
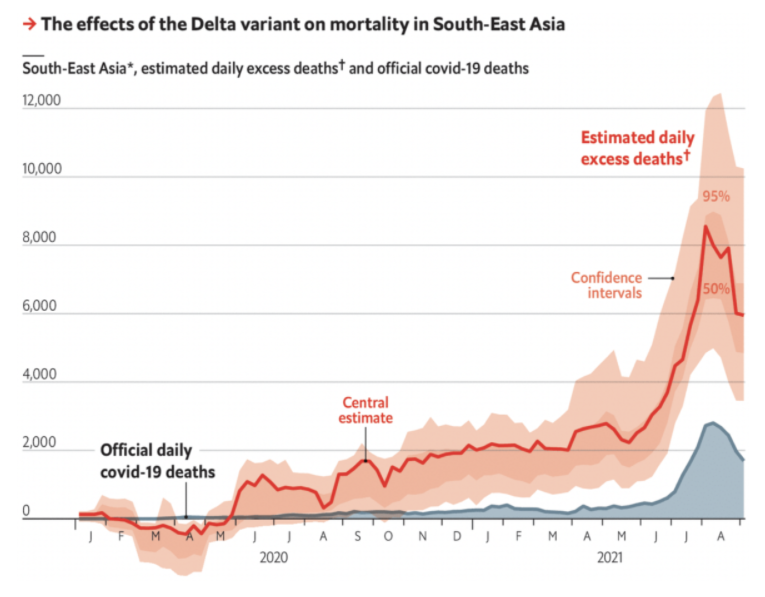
As covid-19 has spread around the world, people have become grimly familiar with the death tolls that their governments publish each day. Unfortunately, the total number of fatalities caused by the pandemic may be even higher, for several reasons. First, the official statistics in many countries exclude victims who did not test positive for coronavirus before dying—which can be a substantial majority in places with little capacity for testing. Second, hospitals and civil registries may not process death certificates for several days, or even weeks, which creates lags in the data. And third, the pandemic has made it harder for doctors to treat other conditions and discouraged people from going to hospital, which may have indirectly caused an increase in fatalities from diseases other than covid-19.
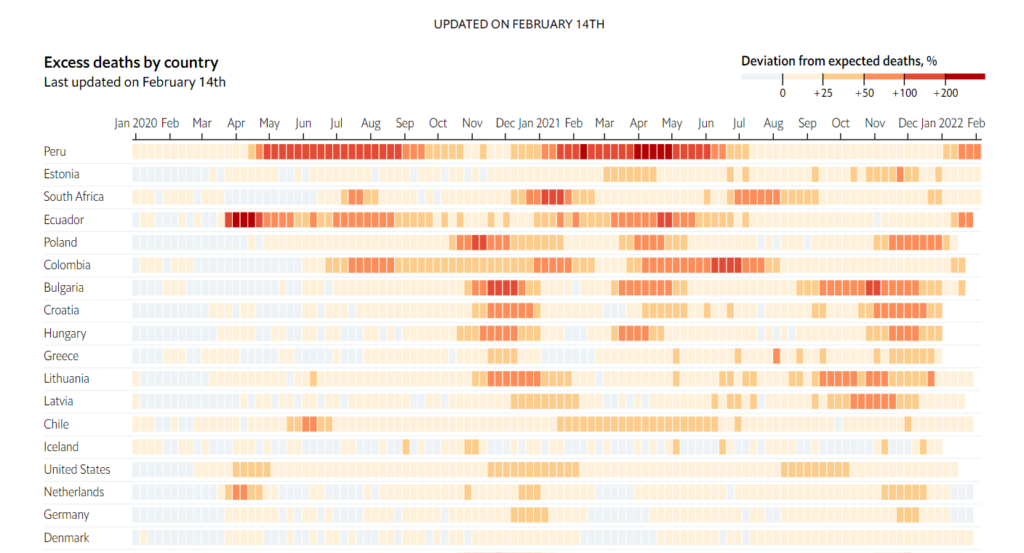
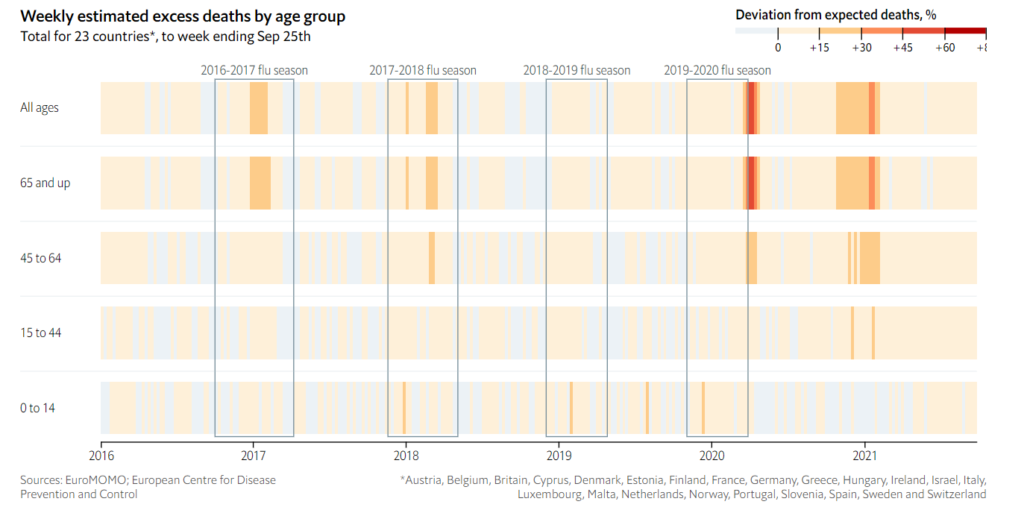
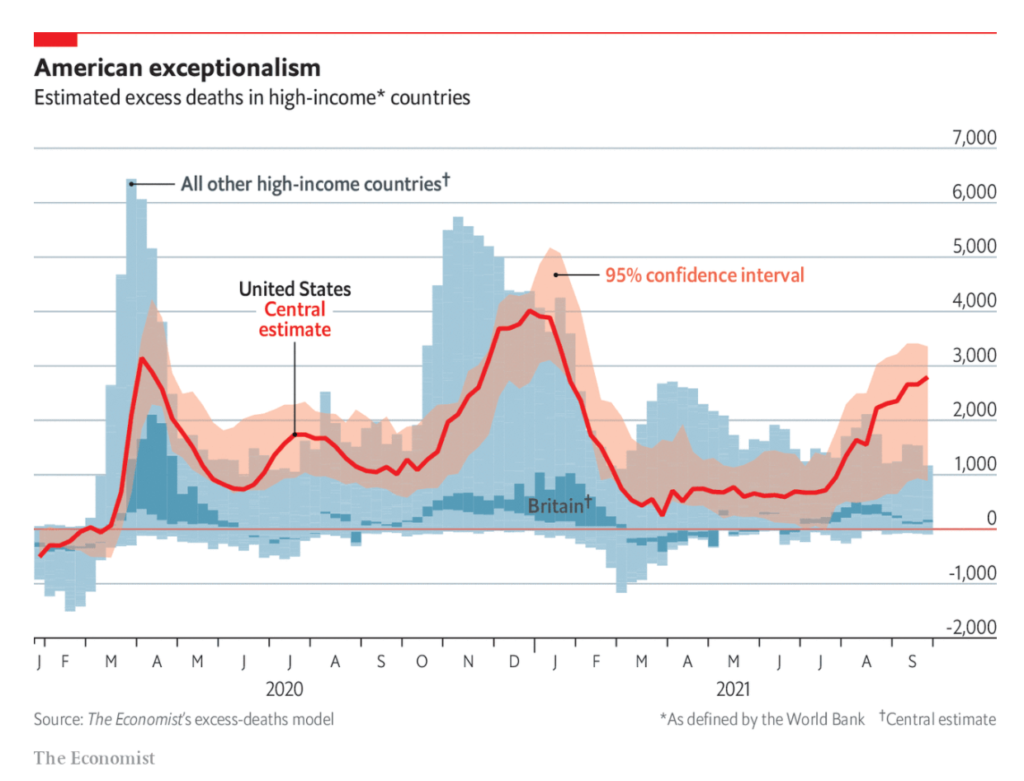
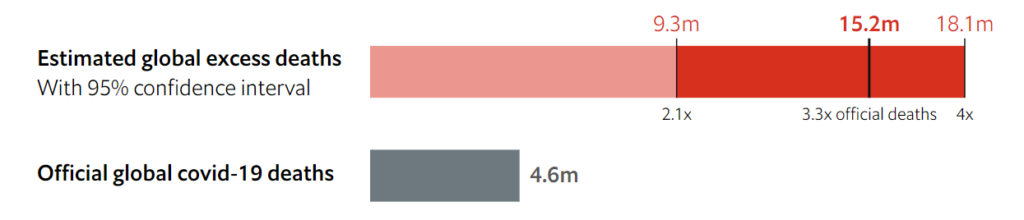
One way to account for these methodological problems is to use a simpler measure, known as “excess deaths”: take the number of people who die from any cause in a given region and period, and then compare it with a historical baseline from recent years. We have used statistical models to create our baselines, by predicting the number of deaths each region would normally have recorded in 2020 and 2021.
Many Western countries, and some nations and regions elsewhere, regularly publish data on mortality from all causes. The table below shows that, in most places, the number of excess deaths (compared with our baseline) is greater than the number of covid-19 fatalities officially recorded by the government. The full data for each country, as well as our underlying code, can be downloaded from our GitHub repository. Our sources also include the Human Mortality Database, a collaboration between UC Berkeley and the Max Planck Institute in Germany, and the World Mortality Dataset, created by Ariel Karlinsky and Dmitry Kobak.
Publication Date: last updated 13 May 2022
Publication Site: The Economist