Graphic:
Excerpt:
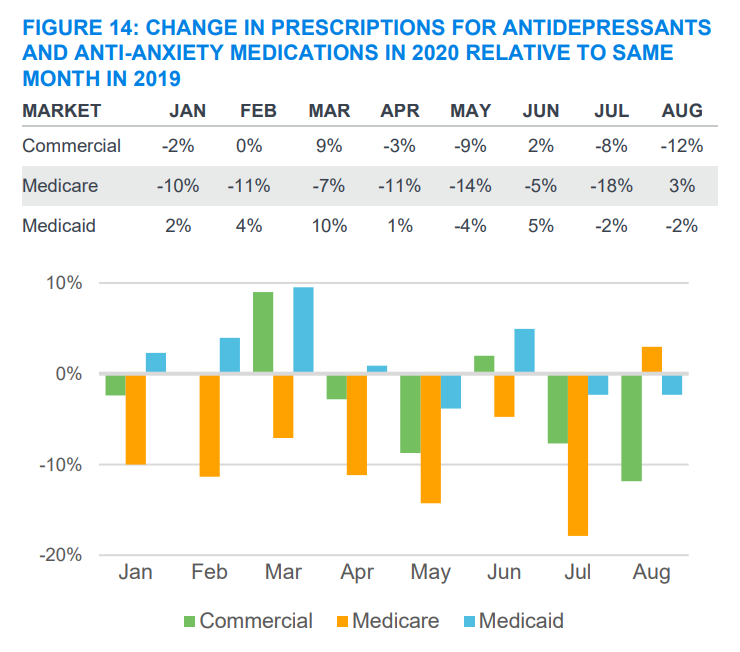
Like utilization for non-Covid-related physical health care, utilization of mental health services dropped significantly when COVID-19 took hold in the United States in early 2020. However, in evaluating those dips, the use of care involving mental health conditions fell less than other kinds of care.
People with a mental health diagnosis were less willing to forego care during COVID-19’s peak. When restrictions began to be lifted in June 2020, visits to primary care offices by those with a mental health diagnosis actually rose above 2019 levels.
With the exception of Medicare beneficiaries, when remote health care utilization was factored into individuals’ overall behavioral health care utilization numbers, there were primarily year-over-year increases across all insured populations. Mental health care utilization increased among the Medicaid population between 2019 and 2020, and only decreased by 1% in March and May among the commercially insured population.
Publication Date: 16 March 2021
Publication Site: Well Being Trust